 |
| Cutaneous Infections | Periungual Telangiectasia | ||
| Abstract | Candida Infections | Erysipelas-Like Erythema | |
| Pseudomonas Infections | |||
| Introduction | Dermatophytosis | Other Skin Markers | |
| Dermal Manifestations | Yellow Nails | ||
| Genetic Considerations | Diabetic Thick Skin | Diabetic Bullae | Diabetic Neuropathy |
| Alopecia Areata | Yellow Skin | Granuloma Annulare | Autonomic Neuropathy |
| Porphyria Cutanea Tarda | Vascular Manifestations | Necrobiosis Lipoidica | Motor Neuropathy |
| Myxedema | Macroangiopathy | Lichen Planus | Sensory Neuropathy |
| Lipid Abnormalities | Diabetic Dermopathy | Bullous Pemphigoid | |
| Biochemical Considerations | Pigmented Purpura | Fat Hypertrophy |
Diabetes mellitus is a common condition which frequently has
skin manifestations. The attachment of glucose to protein may
result in a profound effect on structure and function of that
protein, and account for clinical manifestations of the disease.
It has been suggested that increased crosslinking of collagen in
diabetic patients is responsible for the fact that their skin is
generally thicker than that of non-diabetics. Advanced
glycosylation end products are probably responsible for yellowing
of skin and nails. Increased viscosity of blood due to stiff red
blood cell membranes results in engorgement of the post-capillary
venules in the papillary dermis, detected as erythema of the
face, or periungual erythema. It is suggested that these skin
changes may eventually be used as a reflection of the patient's
current as well as past metabolic status. ![]()
Skin manifestations in diabetes mellitus are common and
expressed in numerous forms. If one considers metabolic effects
on microcirculation and changes in skin collagen, prevalence
approaches 100 percent. Findings range from the presenting
manifestations of the disease to signs of long term involvement,
from the mundane to indications of serious, even life-threatening
problems. For all of these, recognition is the key to treatment
and/or prevention. This review of cutaneous manifestations of
diabetes groups findings according to presumed pathophysiology.
Since the pathophysiology is not always known, some less common
findings are discussed separately at the end.![]()
In 1968 Rahbar published the observation that patients with
diabetes mellitus have oddly behaving hemoglobin.(1)
This was subsequently demonstrated to be due to non-enzymatic
condensation of glucose with hemoglobin to form stable covalent
adducts. Non-enzymatic glycosylation occurs with many proteins
including hemoglobin, an attachment that results in changes in
the physical and chemical properties.![]()
Glucose in solution exists as a stable pyranose ring in
equilibrium with the open chain aldehyde form. The reaction of
monosaccharides with proteins consists of the covalent linkage of
the double-bonded oxygen of the aldehyde function with an NH2
group, either on the alpha-amino group of the N-terminal amino
acid or on the epsilon-amino group of lysine. This condensation
results in the formation of a Schiff base or aldimine, and is a
reversible reaction. However, following the formation of the
Schiff base, there is an internal reconfiguration of the
molecule, the so called Amadori rearrangement, resulting in
formation of a ketoamine which tends to not revert back to the
Schiff base. The rate of reaction of various carbohydrates with
protein correlates with the extent to which the sugar exists in
the open ring (aldehyde) form.![]()
Following the condensation and reconfiguration, the Amadori
products undergo a series of further reactions with amino groups
on other proteins to form glucose-derived intermolecular
crosslinks. (2) These collagen modifications
result in a color change which has been demonstrated by
spectrophotometric measurement to correlate with diabetic
complications. (3) One of these advanced
glycosylation products, a yellow compound, 2-(2-
furoyl)-4(5)-(2-furanyl)-1H-imidazole, has been identified. (4) Quantitation of another advanced glycosylation
end product in the skin, the amino acid pentosidine, has also
been demonstrated to correlate with a cumulative score of
diabetic complications. (5)![]()
The process of non-enzymatic glycosylation occurs to a minor
extent at normal blood sugar concentrations. This gradual
glycosylation of proteins may be responsible for some of the skin
changes associated with aging, and this process is apparently
accelerated in persons with elevated blood sugars. Most proteins
evaluated seem to be involved by this reaction which results in
changes in the physical and chemical properties. Glucosylation of
the red cell membrane is apparently responsible for the stiffness
of diabetic erythrocytes. (6) Glucosylation of
collagen results in increased stiffness and resistance to
enzymatic degradation, mechanical changes of collagen which are
also characteristic for aging.![]()
Protein glycosylation with changes in tertiary structure and
solubility of proteins could conceivably be responsible for many
of the complications of this disease.![]()
Wolfram's or DIDMOAD syndrome (OMIM )
(diabetes insipidus, diabetes mellitus, optic atrophy, and nerve
deafness). (autosomal recessive and associated with non-immune
complete and selective beta cell destruction and severe and
progressive neuronal loss. Onset of diabetes is often in infancy.
This syndrome appears to be responsive to thiamine. There are no
characteristic skin findings reported. Wolfram syndrome is a rare
inherited disorder that leads to an array of symptoms, including
diabetes mellitus and blindness. More important, the syndrome's
victims usually suffer from severe nervous system abnormalities
that can be accompanied by behavior problems, psychiatric
hospitalizations and--in 25 percent of cases--suicide attempts.
Linkage analysis indicates that the likely location of the
Wolfram gene is the short arm of chromosome 4. Between one in
50,000 to 100,000 people in this country inherit Wolfram
syndrome. Although the syndrome itself is rare, experts estimate
that about 1 in 100--or as many as 2.5 million Americans--possess
a single copy of the mutated gene. Because these individuals, as
well as close relatives of people with Wolfram syndrome,
experience higher-than-normal rates of psychiatric illness. ![]()
Maturity onset Diabetes of Youth (MODY) syndrome (OMIM ).
Variants of this syndrome may be very common in American blacks
and individuals from India. In some families inheritance is
autosomal dominant. Chlorpropamide-alcohol flushing may be a
marker for this form. ![]()
Hemochromatosis (OMIM ).
This is associated with the development of diabetes, and the
autosomal recessive gene causing hemochromatosis is located
within the major histocompatibility complex and is associated
with HLA antigens A3 and B14. Patients with this syndrome often
have insulin resistance in association with other manifestations
of iron overload (bronzing of the skin, hepatomegaly,
and cirrhosis). Affected asymptomatic individuals can now be
identified even prior to increased serum ferritin, since the one
in four siblings HLA identical to a hemochromatotic sibling are
almost always homozygous for the involved gene. The gene causing
hemochromatosis is very common in the general population (almost
10%); thus, approximately 2.5% of offspring of a patient with
hemochromatosis will develop hemochromatosis. The sequelae of
iron overload are preventable with simple phlebotomy, and
therefore it is important to screen all first degree relatives of
patients with hemochromatosis for abnormal iron metabolism (e.g.,
transferrin saturation, ferritin levels). ![]()
In secondary forms of iron overload including transfusional
hemosiderosis, alcoholic cirrhosis, thalassemia, sideroblastic
anemia, and porphyria cutanea tarda (OMIM ),
iron accumulates in the reticuloendothelial system initially, but
with increasing amounts of total body iron, excessive iron
deposits eventually accumulate in parenchymal cells throughout
the body producing a picture indistinguishable from hereditary
hemochromatosis. Subnormal activity of hepatic uroporphyrinogen
decarboxylase is responsible for the derangement of porphyrin
biosynthesis in both sporadic and familial porphyria cutanea
tarda, but the enzymatic defect is not clinically expressed in
the absence of hepatic siderosis Pedigree studies support the
hypothesis that HLA-linked hemochromatosis alleles are far more
common inpatients with sporadic porphyria cutanea tarda than in
individuals in the general population and may be responsible for
the hepatic siderosis associated with most cases of sporadic
porphyria cutanea tarda. ![]()
In a study of the skin manifestations of idiopathic
hemochromatosis in 100 cases, there was a high frequency of
ichthyosis-like states and koilonychia. In 50 cases with treated
and non-treated groups, histological siderosis and clinical skin
pigmentation were found to decrease post-phlebotomy whereas
melanosis did not. Siderosis of eccrine sweat glands provided a
probable diagnosis of the disease. Necrobiosis lipoidica and a
black keratinous cyst have also been reported. ![]()
Porphyria cutanea tarda, clinical (1 ,
2 ) . The latter is more commonly seen, producing
photosensitivity in the exposed areas, e.g., bullae on the dorsa
of the hands, showing pink urine with the Wood's lamp
examination. This condition usually is seen in liver damage from
barbiturates, contraceptive pills, estrogens, alcohol or diabetes. The treatment is phlebotomy.![]()
Autoimmune polyendocrinopathy-candidiasis-ectodermal dystrophies
an autosomal recessive disease characterized by a variable
combination of (1) failure of the parathyroid glands, adrenal
cortex, gonads, pancreatic beta cells, gastric parietal cells,
and thyroid gland with associated myxedema,
and hepatitis; (2) chronic mucocutaneous candidiasis; and (3)
dystrophy of dental enamel, nail pitting, alopecia areata,
vitiligo and ocular keratopathy. This disease has many names, one
being autoimmune polyglandular disease Type I. ![]()
| The photographs at the right illustrate several of the more common autoimmune conditions seen in autoimmune polyglandular disease Type I |  |
 |
 |
 |
In a recent study of 68 patients form 54 families, the
clinical manifestations varied greatly and included from one to
eight disease components, 63 percent of the patients having three
to five of them. The initial manifestation was oral candidiasis
in 41 patient (60%). The earliest endocrine component appeared at
19 months to 35 years of age. Eight patients (12%) had
insulin-dependent diabetes mellitus, with the age at onset
ranging from 4.1 to 37 years. Nine patients had vitamin B12
deficiencies that began at the ages of 6.1 to 47. Two female
patients had non-goitrous hypothyroidism; no other patient had
any thyroid autoimmune disease. ![]()
All 68 patients had oral candidiasis at least periodically;
this condition first appeared at ages ranging from one month to
21 years. In six patients the candidiasis was very mild and
disappeared spontaneously for as long as several years, but it
always recurred. Other patients had chronic hypertrophic lesions,
atrophic lesions, or both. Ungual candidiasis was present in 48
patients, and dermal candidiasis in six. The lesions were usually
located on the hands and face. Four patients had esophagitis that
was diagnosed by endoscopy, with stricture in one. Eleven other
patients reported periods of retrosternal pain that resolved
within days after the initiation of oral antifungal therapy.
Ketoconazole 200 mg PO daily was effective in a double-blind
trial; all six ketoconazole-treated patients showed clear
clinical and mycological improvement, of oral and nail
involvement. Death due to metastatic squamous cell carcinoma of
the oral mucosa has been reported. ![]()
77% of patients had hypoplasia of the dental enamel that had
begun at birth or during the first seven years. 2% had pitted
dystrophy of the nails. The pits were 0.5 to 1 mm in diameter and
affected several nails; The surface of the nail was otherwise
smooth. ![]()
The relationship between insulin resistance and acanthosis
nigricans is especially clear in the context of normal and
disordered insulin metabolism. Insulin facilitates the uptake of
glucose into most cells, regulates fat and protein metabolism,
and promotes DNA synthesis and cell growth. Many of these
functions are thought to be modulated by the binding of insulin
to the insulin receptor, a membrane glycoprotein with intrinsic
tyrosine-kinase activity. In addition, insulin can bind to the
receptors composed of insulin-like growth factors. Insulin-like
growth factors are peptides with structures homologous to that of
insulin, and like insulin, these peptides have growth-promoting
effects. In recent studies it has been suggested that the
growth-promoting effects of insulin at low concentrations are
medicated by "classic" receptors, whereas effects at
high concentrations are mediated by insulin-like growth factor
receptors.![]()
High plasma levels of insulin are thought to contribute to the
development of acanthosis nigricans. Evidence for this hypothesis
include the following observations: classic insulin receptors and
insulin-like growth factor receptors have been identified in
cultured human fibroblasts and keratinocytes. Localized
acanthosis nigricans has been noted at sites of subcutaneous
administration of insulin for the treatment of diabetes mellitus.
Finally, many of the conditions associated with acanthosis
nigricans have been linked to the presence of some form of
insulin ![]() resistance.
resistance.
| Alström syndrome | Ataxia-telangiectasia | Bloom syndrome |
| Capozucco syndrome | Crouzon's disease (craniofacial dysostosis) | Lawrence-Seip syndrome (total lipodystrophy) |
| Leprechaunism (70) | Prader-Willi syndrome | Rabson's syndrome |
| Rud's syndrome | Syndrome of acral hypertrophy and muscle cramps | Polycystic ovary disease (Stein-Leventhal syndrome) |
| Acromegally |   |
|||||
| Others Not Represented Here |
|
| Nicotinic acid | Diethylstilbestrol | Glucocorticoids |
In the pre-insulin era the prevalence of common pyodermas such
as furunculosis, carbunculosis, and erysipelas was much higher
for diabetics than for their non-diabetic counterparts. (7) Today, these infections do not seem to result in
much morbidity and diabetics do not even appear to have an
increase in the prevalence of skin infection. (8)
However, there are several infections which characteristically
occur in persons with diabetes mellitus, and some threaten life
and limb.![]()
Yeast infections are common in diabetic patients. Involvement
of the glans penis and of the vulva appear common in type II
diabetes. Vaginal candidiasis is almost universal among women
with long term diabetes, and yeast infections may even be the
presenting manifestation of diabetes.(9)![]()
Vulvo-vaginal candida infection is an especially common
problem for the diabetic woman. (10) It is a
common cause of pruritus vulvae during glycosuria. Presenting
signs include vulvar erythema which may be accompanied by
fissuring with or without satellite pustules. Vaginitis is
usually accompanied by a white discharge. Traditional treatment
involves normalizing blood sugar, treating both the vagina and
vulva with topical medication. Since these patients often have a
reservoir of Candida in the colon, oral nystatin may also be
administered. Another option for vaginal candidiasis is oral
administration of one dose 150 of mg of fluconazole.![]()
Angular stomatitis due to Candida is a classic complication in
diabetic children and an occasional complication in diabetic
adults. Increased concentrations of salivary glucose reportedly
accounts for its occurrence, (11) but not for
the predilection for younger patients. Clinically it is
appreciated as white, curd- like material which adheres to
erythematous, fissured areas at the angle of the mouth or as
white patches on the buccal mucosa and palate. Diagnosis is
readily confirmed by examination of a potassium hydroxide
preparation. Success in treatment may depend on normalization of
blood sugar and the supplemental use of anticandidal lozenges.![]()
The prevalence of Candida infection of the hands and feet does
not appear to be significantly different for the diabetic
population as compared to controls. (12) When
it does occur, it usually has one of three presentations. Candida
paronychia usually involves the hands but it may occur on the
feet. It often begins at the lateral nail folds as erythema,
swelling, and separation of the fold from the lateral margin of
the nail. Further infection may result in involvement of the
proximal nail fold and separation of the cuticle from the nail.
Moisture trapped in the resultant space favors further growth of
the yeast and repeated episodes of inflammation. At times there
may be a purulent discharge from involved nail fold, a clinical
finding suggesting bacterial paronychia. But the diagnosis of
yeast infection can usually be established by performing a KOH
preparation on extruded serous material from this space.![]()
Candida infection of the web spaces usually involves the 3-4
web space of the hands or the 4-5 web-space of the toes. This
area has a tendency to retain moisture due to occlusion from
apposing surfaces of skin. Presumably the increased sugar content
of the skin encourages the establishment of this infection. The
clinical appearance is a white patch of skin, often with central
peeling. Toe web space involvement is often mistaken for a
dermatophyte infection, but the diagnosis can be confirmed on
potassium hydroxide preparation.![]()
The third presentation of Candida infection of the extremities
is involvement in the toe nail plates. Although dystrophic toe
nails are often assumed to be the result of dermatophyte
infection, nail plate cultures demonstrate the pathogen to be
Candida species about five percent of the time. One needs to be
careful about making the diagnosis of primary Candida infection,
however, because cultures may only reflect contaminants or
secondary involvement.Clinically, nail plate infections with
either dermatophyte or Candida sp. present with distal yellowing
or whitening and thickening of the toe nail. Living tissue does
not appear to be involved. If there is a special risk to the
diabetic host to have this nail plate infection, it has not been
demonstrated.![]()
 |
Chronic Candidiasis of the fingernails |
 |
Hyperglycemia can allow usually nonpathogenic organisms to establish an infection in traumatized skin, occasionally resulting in gangrene and loss of limb. |
Diabetic patients with leg ulcers, or non-healing surgical
wounds, especially those of the lower extremities, may have a
complicating Phycomycetes infection. Such an infection should be
suspected when lower extremity ulcers or post-traumatic lesions
are not responding to therapy. Diagnosis can be confirmed by
culture and by histologic demonstration of fungal elements
invading vascular channels.![]()
Patients with uncontrolled diabetes with ketosis may be
predisposed to deep mycotic infections such as the rare but
serious forms of mucormycosis. The characteristic presentation is
black crusting or pus on the turbinates, septum, or palate.
Without treatment the infection may extend to the maxillary and
ethmoid sinuses, the palate, and the orbit. Cerebral involvement
occurs in about two thirds of these patients. (13)
Treatment consists of correction of acid-base imbalance,
aggressive debridement of necrotic tissue, and intravenous
amphotericin.![]()
Malignant external otitis, an uncommon, but serious, infection
of the external ear canal by Pseudomonas, characteristically
presents as and severe external ear canal pain and purulent
discharge in an elderly diabetic patient. (14,15) The infection is thought to begin as a
cellulitis of the ear canal, but natural cleavage planes allow
progression through the osseous cartilaginous junction. With
further extension the cranial nerves may be involved, especially
the facial nerve. About half the affected individuals die of this
infection. Treatment of choice consists of surgical debridement
and administration of anti-pseudomonas antibiotics. ![]()
Much more common than malignant external otitis, however, is
Pseudomonas infection of the toe web spaces or colonization under
the toenails. Often, persons who have onychomycosis develop a
lifting of the nail plate form the bed (onycholysis). The
resulting space between plate and bed may become colonized with
Pseudomonas resulting in a green discoloration of this area. ![]()
Pseudomonas may cause web space infection on the feet similar
to that due to dermatophytosis, but this assumption may be
incorrect. The differential diagnosis includes candidiasis,
infection due to Pseudomonas, but a Wood's lamp examination often
yields a green fluorescence. Soaks with dilute vinegar may
eradicate superficial infection, with more advanced cellulitis,
oral Ciprofloxacin appears to be the treatment of choice. ![]()
Although dermatophyte infections are probably not more common
in the diabetic population, (16) they are of
special concern. Toe web space infections may lead to
inflammation and fissuring that can serve as a portal of entry
for bacterial infection in a compromised diabetic foot. The
oxygen demand of the subsequent inflammation may exceed the
ability of the diabetic microcirculation, leading to gangrene. It
is for that reason that tinea pedis should be aggressively
managed in patients with neurovascular compromise.![]()
Involvement of the toe-nails by dermatophytes (onychomycosis)
is common among elderly diabetics as it is in the population at
large. The infection itself is of little consequence, but the
nail dystrophy which results may make proper nail care more
difficult for the patient. Recently the FDA
approved both Itraconazole treatment (200 mg/day for one week a
month for 4 months) and Terbinafine (250 mg/day for 3 months.)![]()
Persons with diabetes tend to have thicker skin than their
non-diabetic counterparts. There are three aspects to this
observation. First, diabetics in general have a clinically
inapparent but measurable increase in skin thickness unassociated
with symptoms and goes unnoticed by patients and physicians.
Second is a clinically apparent thickening of skin involving the
fingers and hands ranging from pebbled skin to scleroderma-like
skin changes. And third is an infrequent syndrome of diabetic
scleredema in which the patient develops markedly thickened
dermis on the upper back region.![]()
The presence of diabetes mellitus is generally associated with
measurably thickened skin. Using pulsed ultrasound, it can be
demonstrated that diabetics have thicker forearm skin than their
age and sex-matched nondiabetic counterparts.(17)
Contrary to the pattern in non-diabetics, skin thickness may
increase with age (apparently associated with increased duration
of diabetes.) Most studies have used the upper extremity skin in
evaluating skin thickness, and it may not be a valid conclusion
that diabetic skin is thickened at other sites. We have also
demonstrated an increased skin thickness on the dorsum of the
feet, but not the back, suggesting that increased skin thickness
is not necessarily universal in diabetes.(18)
It appears to be a safe observation that patients with diabetes
mellitus have thicker skin on their extremities.![]()
Thickening of skin of the hand is a common occurrence, with a
range of manifestation from simple pebbling of the knuckles to
the diabetic hand syndrome. The diabetic hand syndrome consists
of thickened skin over the dorsum of the digits and limited joint
mobility, especially of the interphalangeal joints.(19)
The earliest description of this phenomenon was apparently the
observation that insulin- dependent diabetes was occasionally
complicated by painful stiff hands.(20)
Subsequently, Rosenbloom and Frais described three adolescent
patients with the syndrome of long-standing diabetes mellitus,
restricted joint mobility, thick tight waxy skin, growth
impairment, and maturational delay.(21)
Rosenbloom et al later reported in a study of 309 mostly juvenile
diabetics that 30 percent had joint limitation and one third of
these had thick tight, waxy skin that the examiner could not
tent, mostly involving the dorsum of the hands.(22)
This work has been confirmed by other authors and these
observations have been extended to patients with type II diabetes
mellitus.(23)![]()
More common is simple thickening of the skin on the dorsum of
the hands. At least thirty percent of diabetic patients have hand
skin thickening, and some have demonstrable involvement of the
dorsum of the feet. Clinical clues which suggest such a
thickening include difficulty in tenting the skin, pebbled or
rough skin on the knuckles or periungual region,(24)
and decreased skin wrinkling following immersion in water.(25)![]()
. What is the significance of thick skin on the hands and feet
in diabetes mellitus? The literature suggests that digital
sclerosis (very thick skin) is a marker for retinal microvascular
disease. But there is a spectrum of thickening of the skin which
ranges from that which is only detectable by ultrasound to the
more obvious. For less than digital sclerosis, the significance
of thick skin in diabetes is uncertain at this time.![]()
Scleredema adultorum of diabetes is a syndrome characterized
by a marked increase in dermal thickness on the posterior back
and upper neck in middle aged, overweight, poorly controlled type
II diabetic subjects. It is not recognized a being related to
digital sclerosis, and we found no correlation by ultrasound
measurements of back skin and hand skin thickness. It has a
reported prevalence of 2.5 percent in patients with type II
diabetes.(26) Histologically one finds a
thickened dermis with large collagen bundles that are separated
by wide, clear spaces. There may be increased numbers of mast
cells. (27) There are reports of increased,
normal, and decreased glycosaminoglycans in affected dermis.(28)![]()
Are there any known treatments for the thick skin syndromes?
There is one study which suggests that tight control of blood
sugar helps. Lieberman et al reported that four diabetic patients
with thick skin had a decrease of skin thickness following pump
administration of insulin and achievement of tighter control.(29) In that study skin thickness was measured
ultrasonically on six body areas and the sums of pre- and post-
treatment determinations were compared. However, they did not
report thickness measurements for any one area. There is no known
treatment for diabetic scleredema.![]()
Diabetic skin often has a yellow hue. Traditionally considered
to be carotenemia, recent evaluations indicate that serum
carotene levels are not elevated as they had been years ago when
the standard diabetic diet involved heavy consumption of
vegetables.(30)![]()
One possible cause of yellow skin might be glycosylation end
products. It is known that proteins which have a long turnover
time, such as dermal collagen, undergo glycosylation and become
yellow. One of the advanced glycosylation products which has been
identified, 2-(2-furoyl)-4(5)-(2-furanyl)-1H-imidazole, has a
distinctly yellow hue (see the earlier section on Biochemical
Considerations).![]()
Yellow skin is a common finding among patients with diabetes,
probably best appreciated on the palms and soles because of
sparse competition with melanocytic pigment in these areas. There
is currently no significance associated with this finding other
than that of a time proven observation.![]()
Diabetics have a higher incidence and prevalence of large
vessel disease,(31) and develop myocardial
infarctions and strokes at a much younger age than their
non-diabetic counterparts. Large vessel disease (atherosclerosis)
may also be present in the lower extremities and result in skin
atrophy, hair loss, coldness of the toes, nail dystrophy, pallor
upon elevation, and mottling on dependence. (32)![]()
Microangiopathy is one of the major complications of diabetes
mellitus. The small blood vessel changes affecting the retinal
and renal vasculature are responsible for blindness and kidney
failure Microvascular pathology has also been assumed to play a
role in diabetic neuropathy, and in the so-called diabetic foot.
Microangiopathy is clinically detected by an eye ground
examination which demonstrates the presence of microaneurysms.
More severe involvement may demonstrate hemorrhages, exudates,
and even some devascularized areas as well.![]()
  |
Kyrle's Disease: an uncommon
finding in patient receiving renal dialysis. The skin is extruding collagen in this disorder which is much more prevalent in diabetes. |
The histology of affected diabetic tissue reveals a PAS
positive, thickened capillary basement membrane. Electron
microscopy of skeletal muscle capillaries reveals reduplication
of the basal lamina. The skin has not been thought to be a good
sample source in evaluation of patients microangiopathy because
small blood vessels of the dermis develop less basal lamina
thickening than is found in skeletal muscle (which is also easily
accessed using a needle biopsy).![]()
The structural changes which occur in the microcirculation do
not seem to account for all the full extent of the disease,
leading to the concept of functional microangiopathy. Some
patients with severe microcirculatory problems such as gangrene
of the foot have normal capillaries on skin or skeletal muscle
biopsy. Sluggish microcirculation resulting in micro-venular
dilatation is considered "functional" in that it may be
reversed with improved control of diabetes. The clinical
manifestations associated with this include retinal venous
dilatation, red face, and periungual telangiectasia, all of which
may be very early manifestations of the disease and which may
improve with control of diabetes.![]()
Functional microangiopathy may result from nonenzymatic
glycosylation which affects many blood components including
hemoglobin, red blood cell membrane, fibronectin, fibrinogen, and
platelets. Glucosylation of the red blood cell has been shown to
inhibit the cell pliability and to decrease the ability of this
cell to pass through pores smaller than 7 microns. The lumen of
some capillaries may be as narrow as 3 microns and ordinarily red
blood cells will elongate into a more sausage like configuration
to traverse this loop. Stiffened membranes will certainly inhibit
or limit this passage.![]()
In addition to stiffened red blood cells, diabetics also have
increased plasma concentration of fibrinogen and capillary
leakage leading to loss of albumen and water. There is an
increased tendency for diabetic platelets to aggregate. The end
result is increased whole blood or plasma viscosity and sluggish
microcirculation.![]()
In summary, it appears that microangiopathy can be attributed
to both structural and functional abnormalities in these vessels.
The following discussion will review some of the cutaneous
manifestations which may be linked to this microangiopathy.![]()
Atrophic hyperpigmented macules on the shins, so-called
diabetic dermopathy, has been termed the most common cutaneous
finding in diabetes.(33) It is usually noted as
irregularly round or oval, circumscribed, shallow lesions vary in
number from few to many, which are usually bilateral but not
symmetrically distributed. They are asymptomatic and often
overlooked.![]()
The genesis of these lesions is unclear. Some authors describe
a preceding, distinct, red papular eruption which is independent
of trauma to the skin.(34) However, Lithner has
been able to duplicate these lesions by local thermal trauma.(35) We observe that many patients who develop
these depressed hyperpigmented lesions relate antecedent trauma
or mild pyoderma such as folliculitis. "Diabetic
dermopathy" probably represents post-traumatic atrophy and
post-inflammatory hyperpigmentation in poorly vascularized skin.![]()
Do these lesions represent the cutaneous manifestation of
structural microangiopathy? Histologic characteristics of acute
lesions are edema of the epidermis and papillary dermis,
extravasated erythrocytes and a mild lymphohistiocytic
infiltrate.(36) Older lesions have thick-walled
capillaries in the upper dermis, occasional extravasated
erythrocytes and a positive Perl stain for iron. However, one
electron microscopic study demonstrated only in some patients the
presence of thickened basal lamina.(37) Based
on the available studies, there appear to be structural
components and some suggestion of a functional factors as well.![]()
The significance and prevalence of diabetic dermopathy depends
on the operational definition of this entity. Defined as one or
more spots, the original description reported their presence in
55% of 293 diabetics (65% of males and 29% of females).(38) But with this definition, it has also been
shown to occur in 20% of control patients with normal glucose
tolerance tests.(39) Thus, defining diabetic
dermopathy as one or more spots results in high sensitivity but
low specificity for diabetes. However, in a study which defined
dermopathy as the presence of four or more lesions, they were
absent in non-diabetics and present in about 14% of diabetics
(24% of men and 3% of women).(40) The
multilesional definition also found a high correlation with
retinovascular disease.![]()
Pigmented purpuric dermatosis is a condition involving the
skin on the lower extremities resulting from red blood cell
extravasation from the superficial vascular plexus. It is
characterized by multiple tan to reddish small macules (so-called
cayenne pepper spots) which coalesce into tan to orange patches.
It often extends down to involve the ankles and the dorsum of the
feet. It was described as a manifestation in older diabetic
patients, about half of whom had diabetic dermopathy.(41) In most of these patients, cardiac
decompensation with edema of the legs was determined to be a
precipitating factor for the purpura. Except for the frequent
association with diabetic dermopathy, this condition appears
clinically consistent with Schambergs disease. Again, with little
insight into the pathophysiology, this condition appears to be a
marker of structural microangiopathy.![]()
The prototype functional microangiopathy is facial
involvement, the so-called rubeosis facei. The intensity of red
coloration which can be appreciated in one's 'complexion' is a
function of the degree of engorgement of the superficial venous
plexus. Hyperglycemia predisposes to sluggish microcirculation
and affected individuals develop a functional microangiopathy
which is clinically evident by venous dilatation.(42)
This venous dilatation can be demonstrated in the eye grounds and
skin. It may be evident in newly diagnosed diabetics and, more
importantly, the vascular engorgement may return to normal when
the blood sugar is controlled. In a prospective study of 150
medical hospital admissions, comparing facial redness (none,
slightly red, or markedly red) with diabetic parameters
(persistent fasting hyperglycemia or a diabetic glucose tolerance
curve), of sixty one patients with diabetes, thirty-six (59%) had
markedly red faces.(43) Because of normal
variation in complexion, this sign is difficult to use as a
marker of functional microangiopathy.![]()
One may directly examine the skin to survey the superficial
microcirculation. Any area of skin may be examined, but because
nailfold capillary loops are in a horizontal axis relative to the
skin surface, this area offers an excellent view of the entire
microvascular loop. In order to see past the stratum corneum, it
is helpful to first apply mineral oil to the skin surface and
wait a few minutes until this layer becomes translucent. One may
use a low power microscope or simply an ophthalmoscope (+40 lens
for 10X magnification). In general, the microcirculation of less
pigmented individuals is often easier to visualize.![]()
One study found venous capillary dilatation in the nail folds
of 49% of seventy-five diabetic patients compared to 10% of
sixty-five controls.(44) It is important to
note that connective tissue diseases may also result in
periungual vessel changes, but that these changes are
morphologically different. In diabetes one sees isolated
homogeneous engorgement of the venular limbs. In connective
tissue diseases, the patterns seen are megacapillaries or
irregularly enlarged loops.(45) ![]()
Venous dilatation of the periungual microcirculation appears
to be an excellent indicator of functional microangiopathy. The
structural changes of this area are probably represented by
venous tortuosity. Thus a newly diagnosed patient is likely do
have simple capillary loops with a dilated venous portion. A long
term diabetic patient who had poor control for a number of years,
but who now has excellent control, may exhibit venous tortuosity
without dilatation. More extensive microangiopathy can be
heralded by small hemorrhages and by drop-out of areas of the
microcirculation.![]()
Another reported phenomenon of microcirculatory compromise in
diabetic patients is the development of well demarcated erythema
on the lower leg or dorsum of the foot that correlates with
radiological evidence of underlying bone destruction, and
incipient gangrene. (46,47)
The condition was at first mistaken for erysipelas (hence the
name erysipelas-like erythema), but there was no associated
pyrexia, elevated erythrocyte sedimentation rate, or
leukocytosis. This erythema would seem to be functional
microangiopathy localized to an area of macrocirculation
compromise.![]()
As pointed out by Lithner, diabetics tend to have yellow
nails.(47) He noted this phenomenon in half of
36 diabetics and in none of nine controls. Our patients have a
similar prevalence of yellow nails, except we also see it
occasionally in elderly controls, and in some patients with
onychomycosis. Although this phenomenon may occur on all the
nails, it is most often evident on the distal aspect of the nail
of the hallux.![]()
What might account for this coloration? Clinically the yellow
color is not usually the result of underlying dermatophytosis.
Similar to the yellow color observed in diabetic skin, yellowing
of the nails probably represents glycosylation end products.
Whereas keratin of the epidermis is only present for one month
before being shed, that of the nail plate may be present for
greater than a year. The protein- glucose reaction presumably
continues to evolve in the aging nail resulting in the most
yellow pigment at the distal aspect of the slowest growing nail.
The presence of the yellow glycosylation end products in the nail
plate has not been confirmed to date, but one study of
fingernails has demonstrated that diabetics have high levels of
fructose-lysine, another marker of nonenzymatic glycosylation.(48)![]()
Clinically one appreciates yellow nails of diabetes best on
examination of the toe-nails. Most diabetic patients have some
aspect of this yellowing. Minimal involvement consists of distal
yellow or yellow-brown discoloration of the hallux nail plate.
Marked involvement consists of canary yellow discoloration of all
toe- and finger-nails. It is not a specific finding in diabetes
mellitus since it can be occasionally observed with normal aging.
Like the yellow hue appreciated generally in the skin of persons
with diabetes, the significance of this observation is
undetermined. The obvious question is whether or not yellow nails
and yellow skin can be used as an quantifiable indicator of the
degree of nonenzymatic glycosylation for other tissues of the
body.![]()
Another curious phenomenon in diabetes mellitus is the
spontaneous appearance of blisters on the extremities (usually
confined to hands or feet). These lesions are not the result of
trauma or infection. They tend to heal without treatment.![]()
On the basis of cleavage level, there appears to be three
types of these blisters. The most common type is spontaneous and
nonscarring. They present as clear, sterile blisters on the tips
of the toes or fingers and less frequently on the dorsal and
lateral surfaces of the feet, legs, hands, and forearms.
Spontaneous healing occurs within 2 to 5 weeks.(49)
These patients were reported to have good circulation to the
affected extremity and tended to have diabetic peripheral
neuropathy. In those patients in whom histopathology has been
performed, there is an intraepidermal cleavage without
acantholysis.(50,51) The
second type of diabetic bullae involves lesions that may be
hemorrhagic and heal with scarring and atrophy.(52,53 The reported cleavage plane is below the
dermoepidermal junction.![]()
A third type described in a case report consists of multiple
tender nonscarring blisters on sun-exposed and deeply tanned
skin, on the feet, legs, and arms. Immunofluorescence and
porphyrin studies were negative. Electron microscopy placed the
cleavage plane at the lamina lucida. (54)![]()
The incidence is 0.3% in diabetics, and it is rare in
non-diabetics. The condition is most common between the second
and fifth decades of life, but it may be seen at any age. 80% of
patients with NLD are women. NLD occurs almost exclusively in
whites. ![]()
between 60 and 65% with NLD will have overt diabetes at the
time of the diagnosis. Of the remainder of patients, about 50%
will show abnormalities when challenged by routine or cortisone
glucose tolerance tests. Another 25% of patients will have a
strong family history of diabetes. This leaves only some 10% of
the total number of patients who lack a diabetic association. ![]()
The primary lesion of NLD is a well-defined, small, firm,
dusky-red papule topped with a fine scale. By slow enlargement or
coalescence, these lesions form indurated plaques that are round
or oblong when small and have an irregular geographic
configuration when larger. The border, which sometimes is
slightly elevated, and the adjoining skin are reddish-blue,
whereas the center is yellow, indicating lipid accumulation. The
size of the lesion may vary from a few millimeters to several
centimeters. The inflammatory process subsides, and the condition
assumes its best recognized, chronic state, that is, the sharply
demarcated sclerotic plaque reminiscent of glazed porcelain. The
glossy atrophic area softens and becomes entirely brown. Through
its surfaces numerous telangiectases and underlying larger blood
vessels can be seen. ![]()
The scale may remain fine or, particularly if ulceration is
imminent, become more prominent and collodion-like. ulceration
occurs in approximately one third of patients regardless of
whether they are diabetic. It is more common in larger lesions
and may follow trauma. ![]()
Lesions of NLD are most frequent on the lower portions of the
legs, the pretibial and medial malleolar areas being the favored
sites. Lesions occasionally appear on the thighs, popliteal
regions, and feet. In 15% of cases other sites are involved in
addition to the legs. These sites include the abdomen, upper
extremities(especially the hands and forearms), and scalp, where
NLD can cause atrophy and alopecia, and the face, including the
eyelids and nose. In rare cases the condition has been noted on
the heels or penis. necrobiosis lipoidica diabeticorum also has
developed in scars and at sites of scleroderma and BCG
vaccinations. Even when the lesions appear elsewhere on the body,
the legs generally are also involved. ![]()
except when they are ulcerated, the papules and plaques are
generally asymptomatic. The occasional patient will have
pruritus, burning, or tenderness. Pain, however, is a frequent
companion of ulceration. Some patients report partial or complete
anesthesia of the affected sites, suggesting local nerve
dysfunction. ![]()
As many as one in five lesions will resolve spontaneously, the
time required for improvement varies from 3 to 4 years. ![]()
Treatment: The physician should stress the probability of
localization of lesions to the low part of the legs, the absence
of contagion, lack of malignant degeneration, and the possibility
that some areas will heal spontaneously. In patients with overt
diabetes, adequate follow-up tests for urine and blood glucose
levels are important. ![]()
The lower parts of the legs should be protected from trauma.
Patients should be advised to avoid potentially traumatizing
situations such as certain sports and they should wear
knee-length stockings or shin pads for protection. ![]()
In general, although many treatments have been touted, they
have little in the way of proven efficacy, and should probably be
reserved for symptomatic relief. ![]()
Topical steroids under occlusion has been used but has not
been subjected to double-blind studies. Dermajet delivery of
triamcinolone acetonide (TMC) has shown improvement in an open
study and intralesional injection of 0.1 cc of TMC, 2.5 mg/ml,
perilesionally at 1 cm intervals has been suggested for active
plaques. Clofazimine 200 mg/day cleared 6/10 patients, of 13
patients who remained on treatment for more than one month, eight
improved ![]()
Necrobiosis lipoidica has been seen in Ehler's-Danlos
Syndrome, type VIII (OMIM )
as well as Ataxia-Telangiectasia (Thibaut )![]()
Necrobiosis lipoidica diabeticorum (NLD) is an uncommon
manifestation of diabetes mellitus, occurring in about 0.3% of
these patients.(55) This skin manifestation is
not pathognomonic for diabetes mellitus since less than two
thirds of patients with necrobiosis lipoidica are diabetic.
Necrobiosis lipoidica has been documented to occur prior to the
onset of diabetes mellitus.(56) Certainly any
patient who presents with necrobiosis lipoidica should be
evaluated for diabetes.![]()
The initial lesions of NLD begin as well-circumscribed
erythematous papules. Evolving radially, the sharply defined
lesions have depressed, waxy, yellow-brown, atrophic
telangiectatic centers through the underlying dermal vessels can
be visualized. The periphery is slightly raised and erythematous
and there may be partial or complete anesthesia of the lesion.(57) Ulceration is reported in about one third of
leg lesions, mostly in large lesions following minor trauma.
Lesions of NLD sometimes spontaneously resolve, but more often
they do not. They seem to occur and persist independent of degree
of control of hyperglycemia.![]()
Whereas most lesions of NLD occur on the legs, about 15
percent of lesions are found elsewhere, including on the hands,
forearms, abdomen, face, or scalp. When necrobiosis lipoidica
occurs in areas other than the lower extremities, the patient is
less likely to have diabetes mellitus.(58)![]()
The histopathology of NLD reveals neutrophilic necrotizing
vasculitis in early lesions.(59 With
progression there is collagen degeneration and destruction of
adnexal structures. Lesions evolve through granulomatous and
sclerotic stages, with most of the sclerosis occurring in the
lower reticular dermis. The upper dermis contains fatty deposits
that give the lesions their yellow color.![]()
Electron microscopy of necrobiosis lipoidica reveals striking
changes involving dermal blood vessels consisting of focal
degeneration of the endothelial cells lining the
microvasculature.(60) These cells have electron
lucency and loss of intracellular organelles.![]()
Treatment is used to arrest the progression of the disease.
This is most commonly achieved by application of high potency
topical steroids or intralesional injection of steroids into the
active margin. Other agents reported include pentoxifylline, high
dose oral nicotinamide(61), aspirin and
dipyridamole(62,63,64) Currently the most impressive therapeutic
option may be oral corticosteroids. Five weeks of oral
corticosteroid treatment was described as resulting in complete
disease cessation for all of six patients treated.(65).
Since the pathophysiology of necrobiosis is not understood, it is
difficult to design rational therapy.![]()
It has been suggested that nonmyelinated nerve fibers, such as
those of the autonomic nervous system, may be the first nervous
tissue affected in diabetics.(66) In clinical
practice, evidence of autonomic neuropathy is common as
manifested by disturbance of sweating (usually anhidrosis) of the
feet. Occasionally patients complain of over-sweating elsewhere,
a compensatory mechanism for loss of the ability to temperature
regulate in the involved area. It has also been reported that
autonomic neuropathy (as measured by quantitation of the sweating
deficiency) correlates well with the severity of sensory
neuropathy.(67) One might safely assume that
patients who have diabetic sensory neuropathy also have
accompanying autonomic involvement.![]()
The clinical manifestations of peripheral autonomic neuropathy
vary from absence of symptoms to complaints that the feet are
abnormally cold, burning, or pruritic. But there is also a
problem due to absence of sweating. Perspiration on the feet
maintains hydration of the stratum corneum: callosities without
hydration tend to become brittle and may fissure serving as a
portal for infection. Thus symptoms and signs of autonomic
peripheral neuropathy in the diabetic patient indicate the need
for extra attention to foot care. ![]()
Diabetic motor neuropathy most often affects the foot. The
clinical presentation is wasting of the interosseous foot muscles
resulting in two major mechanical problems. The foot tends to
splay upon weight bearing, resulting in a wider foot. The toes
tend to draw upward, and the plantar fat pads move forward
leaving the metatarsal heads riding on the plantar skin without
the benefit of padding.![]()
Motor neuropathy may appear suddenly or occur gradually over
several years. Acute and reversible motor neuropathy may follow
an episode of ketoacidosis,(68) or as the
result of insulin excess. More usual is an insidious progression
of motor nerve deterioration over many years.![]()
Motor neuropathy in diabetes mellitus is almost always
accompanied by a sensory involvement. Changes in the shape of the
foot follow the imbalance of its internal musculature and result
in ill-fitting shoes. If the changes go unnoticed, the patient
may continue to wear shoes which can now traumatize the foot.
Because of the accompanying sensory loss, displacement of the
plantar fat pads can result in uncushioned weight bearing at the
metatarsal heads. Callosities and eventually ulceration of the
weight-bearing skin or of the skin being rubbed by the now ill
fitting shoes result (neuropathic ulcers). The presence of motor
neuropathy of the foot often necessitates the use of special
widened shoes with molded inserts to redistribute weight bearing,
to accommodate and to protect the compromised foot.![]()
Diabetics often develop sensory neuropathy on the feet,
especially with long-standing disease. The clinical presentation
usually involves tingling and numbness starting in the toes. The
level of neuropathy may vary from mild numbness of the distal
toes to profound anesthesia and neuropathic ulcers. Thermal
sensitivity is also affected. (69)![]()
What is the clinical significance of sensory neuropathy?
Although tingling and numbness tend to be the complaint, the lack
of sensation may allow trauma to go unnoticed and result in a
traumatic ulceration. Depending upon the status of the
microcirculation, these ulcers may present difficult therapeutic
problems. Neuropathic patients who walk barefoot may sustain
damage when during routine ambulation because they have
inadequate sensation to withdraw the foot when it encounters
noxious stimuli. Occasionally this unsensed trauma during
ambulation results in fracturing the bones of the feet,
eventuating into a Charcot foot.![]()
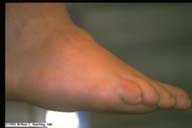 |
Charcot Foot. This patient, with diabetic motor and sensory neuropathy, developed multiple midfoot fractures while running a short distance barefoot. The result is a misshapen foot as seen here. |
Patients with sensory neuropathy need to be instructed to make
sure their shoes are devoid of foreign objects before the shoes
are worn. As simple as it sounds, patients who do not follow this
rule occasionally sustain severe damage by wearing shoes which,
unknown to them, had objects (especially children's toys)
included.![]()
Other Conditions associated with Diabetes
Diabetes Mellitus is a common ailment and virtually all
persons with diabetes develop skin manifestations of this
disease. Many of these manifestations, especially the more common
ones, might be explained on the basis of the attachment of
glucose to proteins, and the subsequent metabolism of this
combination, which results in changes in structure, function, and
color. Hopefully, the common skin findings described here may
eventually be used as indicators of the patient's current and
past metabolic status.![]()
(1)Rahbar S: An abnormal hemoglobin in red
cells of diabetics. Clin Chim Acta 22:296-298, 1968.![]()
(2)Brownlee M, Vlassara H, Kooney A, Ulrich P,
Cerami A: Aminoguanidine prevents diabetes- induced arterial wall
protein cross-linking. Science 232:1629-1632, 1986![]()
(3)Delbridge L, Ellis CS, Robertson K,
Lequesne LP: Non-enzymatic glycosylation of keratin from the
stratum corneum of the diabetic foot. Br J Dermatol 112:547-554,
1985.![]()
(4)Pongor S, Ulrich PC, Benesath FA, Cerami A:
Aging of proteins: Isolation and identification of a fluorescent
chromophore from the reaction of polypeptides with glucose. Proc
Nat Acad Sci USA 81:2684-8, 1984.![]()
(5)Sell DR, Lapolla a, Odetti P, Fogarty J,
and Monnier VM: Pentosidine formation in skin correlates with
severity of complications in individuals with long-standing IDDM.
Diabetes 41:1286-1292, 1992.![]()
(6)Otsuji S, Kamada T: Biophysical changes in
the erythrocyte membrane in diabetes mellitus. Rinsho Byori
30:888-897, 1982.![]()
(7)Greenwood AM: A study of the skin in 500
diabetics. JAMA 89:774-776, 1927![]()
(8)Edwards JE, Tillman DB, Miller ME, Pitchon
HE: Infection and diabetes mellitus. West J Med 130:515-521,
1979.![]()
(9)Muller SA, Winkleman RK: Necrobiosis
lipoidica diabeticorum: A clinical and pathological investigation
of 171 cases. Arch Dermatol 93:272-281, 1966.![]()
(10)Sonck CE, Somersalo O: The yeast flora of
the anogenital region in diabetic girls. Arch Dermatol
88:846-852, 1963. ![]()
(11)Knight L, Fletcher J: Growth of Candida
albicans in saliva: Stimulation by glucose associated with
antibiotics, corticosteroids, and diabetes mellitus. J Infect Dis
123:371-377, 1971.![]()
(12)Lugo-Somolinos A, Sanchez JL: Prevalence
of dermatophytosis in patients with diabetes: J Am Acad Dermatol
26:408-410, 1992.![]()
(13)Tomford JW, Whittlesey D, Ellner JJ,
Tomashefski JF: Invasive primary cutaneous phycomycosis in
diabetic leg ulcers. Arch Surg 115:770-771, 1980.![]()
(14)Petrozzi JW, Warthan TL: Malignant
external otitis. Arch Dermatol 110:258-260, 1974.![]()
(15)Wilson DF, Pulec JL, Linthicum FH:
Malignant external otitis. Arch Otolaryngol 93:419-422, 1971.![]()
(16)Alteras I, Saryt E: Prevalence of
pathogenic fungi in the toe-webs and toe-nails of diabetic
patients. Mycopathologia 67:157-159, 1979.![]()
(17)Collier A, Matthews AM, Kellett HA,
Clarke BF, Hunter JA: Change in skin thickness associated with
cheiroarthropathy in insulin dependent diabetes mellitus. Br Med
J 292:936, 1986.![]()
(18)Huntley AC, Walter RM Jr: Quantitative
determination of skin thickness in diabetes mellitus:
relationship to disease parameters. Journal of Medicine, 1990,
21(5):257-64.![]()
(10)Brik R, Berant M, Vardi P: The
scleroderma-like syndrome of insulin-dependent diabetes mellitus.
Diab Metab Rev 7:121-128, 1991.![]()
(20)Lundbaek, K: Stiff hands in long term
diabetes. Acta Med Scand 158:447-451, 1957. Rosenbloom AL, Frais
JL: Diabetes mellitus, short stature and joint stiffness - a new
syndrome. Clin Res 22:92A, 1974.![]()
(21) Rosenbloom AL, Frais JL: Diabetes
mellitus, short stature and joint stiffness - a new syndrome.
Clin Res 22:92A, 1974.![]()
(22)Rosenbloom AL, Silverstein JH, Lezotte
DC, Richardson K, McCallum M: Limited joint mobility in childhood
diabetes mellitus indicates increased risk for microvascular
disease. N Engl J Med 305:191-198. 1981.![]()
(23)Fitzcharles MA, Duby S, Wadell RW, Banks
E, Karsh J: Limitation of joint mobility (cheiroarthropathy) in
adult noninsulin-dependent diabetic patients. Ann Rheum Dis
43:251-257, 1984.![]()
(24)Huntley AC: Finger pebbles: A common
finding in diabetes mellitus. J Amer Acad Dermatol 14:612-617,
1986.![]()
(25)Clark CV, Pentland B, Ewing DJ, Clark BF:
Decreased skin wrinkling in diabetes mellitus. Diabetes Care
7:224-227, 1984.![]()
(26)Cole GW, Headley J, Skowsky R: Scleredema
diabeticorum: A common and distinct cutaneous manifestation of
diabetes mellitus. Diabetes Care 6:189-192, 1983.![]()
(27)Cohn BA, Wheeler CE, Briggamon RA:
Scleredema adultorum of Buschke and diabetes mellitus. Arch
Dermatol 101:27-35, 1970.![]()
(28)Konohana A, Kawakubo Y, Tajima S,
Kitamura K, Nishikawa T: Glycosaminoglycans and collagen in skin
of a patient with diabetic scleredema. Keio J Med 34:221-226,
1985.![]()
(29)Lieberman LS, Rosenbloom AL, Riley WJ,
Silverstein JH: Reduced skin thickness with pump administration
of insulin [letter]. N Eng J Med 303:940-1, 1980.![]()
(30)Hoerer E, Dreyfuss F, Herzberg M:
Carotenemia, skin color and diabetes mellitus. Acta Diabetol Lat
12:202-207, 1975.![]()
(31)West KM: Epidemiology of diabetes and its
vascular lesions. New York, 1978, Elsevier North-Holland Inc., p
353. ![]()
(32)Haroon TS: Diabetes and skin--a review.
Scott Med J 19:257-267, 1974.![]()
(33)Bernstein JE: Cutaneous manifestations of
diabetes mellitus. Curr Concepts Skin Disord 1:3, 1980.![]()
(34)Bauer M, Levan NE: Diabetic
dermangiopathy. A spectrum including pretibial pigmented patches
and necrobiosis lipoidica diabeticorum. Br J Dermatol 83:528-535,
1970.![]()
(35)Lithner F: Cutaneous reactions of the
extremities of diabetics to local thermal trauma. Acta Med Scand
198:319-325, 1975.![]()
(36)Binkley GW, Giraldo B, Stoughton RB:
Diabetic dermopathy--a clinical study. Cutis 3:955-958, 1967.![]()
(37)Fisher ER, Danowski TS: Histologic,
histochemical, and electron microscopic features of the shin
spots of diabetes mellitus. Am J Clin Path 50:547-554, 1968.![]()
(38)Melin H: An atrophic circumscribed skin
lesion in the lower extremities of diabetics. Acta med Scand
176(Suppl 423):1-75, 1964.![]()
(39)Danowski TX, Sabeh G, Sarver ME, Shelkrot
J, Fisher ER: Shin spots and diabetes mellitus. Am J Med Sci
251:570-5, 1966.![]()
(40)Murphy RA: Skin lesions in diabetic
patients: The "spotted leg" syndrome. Lahey Clin Found
Bull 14:10-14, 1965. ![]()
(41)Lithner F: Purpura, pigmentation and
yellow nails of the lower extremities in diabetes. Acta Med Scand
199:203-208, 1976.![]()
(42)Ditzel J: Functional microangiopathy in
diabetes mellitus. Diabetes 17:388-397, 1968.![]()
(43)Gitelson S, Wertheimer-Kaplinski N: Color
of the face in diabetes mellitus. Observations on a group of
patients in Jerusalem. Diabetes 14:201-208, 1965.![]()
(44)Landau J, Davis E: The small
blood-vessels of the conjunctiva and nailbed in diabetes
mellitus. Lancet 2:731-734, 1960.![]()
(45)Grassi W, Gasparini M, Cervini C:
Nailfold computed videomicroscopy in morpho-functional assessment
of diabetic microangiopathy. Acta Diabetol Lat 22:223-228, 1985.![]()
(46)Lithner F: Cutaneous erythema, with or
without necrosis, localized to the legs and feet--a lesion in
elderly diabetics. Acta Med Scand 196:333-342, 1974.![]()
(47)Lithner F, Hietala S-O: Skeletal lesions
of the feet in diabetics and their relationship to cutaneous
erythema with or without necrosis of the feet. Acta Med Scand
200:155-161, 1976.![]()
(48)Oimomi M, Maeda Y, Hata F, Nishimoto S,
Kitamura Y, Matsumoto S, Hatanaka H, Baba S: Glycosylation levels
of nail proteins in diabetic patients with retinopathy and
neuropathy. Kobe J Med Sci 31:183-188, 1985.![]()
(49)Rocca F, Pereyra E: Phlyctenar lesions in
the feet of diabetic patients. Diabetes 12:220-222, 1963.![]()
(50)Allen GE, Hadden DR: Bullous lesions of
the skin in diabetes (bullous diabeticorum). Br J Dermatol
82:216-220, 1970.![]()
(51)Cantwell AR, Martz W: Idiopathic bullae
in diabetics. Bullosis diabeticorum. Arch Dermatol 96:42-44,
1967.![]()
(52)Kurwa A, Roberts P, Whitehead R:
Concurrence of bullous and atrophic skin lesions in diabetes
mellitus. Arch Dermatol 103:670-675, 1971.![]()
(53)James WD, Odom RB, Goette DK: Bullous
eruption of diabetes mellitus. A case with positive
immunofluorescence microscopy findings. Arch Dermatol
116:1191-1192, 1980.![]()
(54)Bernstein JE, Medinica M, Soltani K,
Griem SF: Bullous eruption of diabetes mellitus. Arch Dermatol
115:324-325, 1979.![]()
(55)Muller SA: Dermatologic disorders
associated with diabetes mellitus. Mayo Clin Proc 41:689-703,
1966.![]()
(56)Ellenberg M: Diabetic complications
without manifest diabetes. JAMA 183:926-930, 1963.![]()
(57)Boulton AJ, Cutfield MB, Abouganem D,
Angus E, Flynn HW, Skyler JS, Penneys NS: Necrobiosis lipoidica
diabeticorum: a clinicopathologic study. J Am Acad Dermatol
18:530537, 1988.![]()
(58)Wilson Jones E: Necrobiosis lipoidica
presenting on the face and scalp. Trans St Johns Hosp Dermatol
Soc 57:202, 1971.![]()
(59)Ackerman AB: Histologic diagnosis of
inflammatory skin diseases. A method by pattern analysis.
Philadelphia, 1978, Lea & Febiger, pp. 424-431.![]()
(60)Heng MCY, Allen SG, Song MK, Heng MK:
Focal endothelial cell degeneration and proliferative
endarteritis in trauma-induced early lesions of necrobiosis
lipoidica diabeticorum. Am J Dermatopath 13:108-114, 1991.![]()
(61)Handfield-Jones S, Jones S, Peachey R:
High dose nicotinamide in the treatment of necrobiosis lipoidica.
Br J Dermatology 118:693-696, 1988.![]()
(62)Eldor S, Diaz EG, Naparstek E: Treatment
of diabetic necrobiosis with aspirin and dipyridamole. N Engl J
Med 298:1033, 1978.![]()
(63)Fjellner B: Treatment of diabetic
necrobiosis with aspirin and dipyridamole. N Engl J Med 299:1366,
1978.![]()
(64)Unge G, Tornling G: treatment of diabetic
necrobiosis with dipyridamole. N Engl J Med 299:1366, 1978.![]()
(65)Petzelbauer P, Wolff K, Tappeiner G:
Necrobiosis lipoidica: treatment with systemic corticosteroids.
Br J Dermatology 126:542-545, 1992.![]()
(66)Martin MM: Involvement of autonomic nerve
fibers in diabetic neuropathy. Lancet 264:560-565, 1953.![]()
(67)Kennedy WR, Sakuta M, Sutherland D, Goetz
FC: Quantitation of the sweating deficiency in diabetes mellitus.
Ann Neurol 15:482-488, 1984.![]()
(68)Brown MJ, Asbury AK: Diabetic neuropathy.
Ann Neurol 15:2-12,1984.![]()
(69)Navarro X, Kennedy WR: Evaluation of
thermal and pain sensitivity in type I diabetic patients. J
Neurol Neurosurg Pshchiatry 54:60-64, 1991.![]()
(70) Robert JJ, TI - Hyperinsulinism
syndromes caused by insulin resistance TT - Exploration des
syndromes d'hyperinsulinisme par resistance a l'insuline. ![]()
(71) Thibaut, S.; Sass, U.; Khoury, A. and
Simonart, J.-M.: Ataxia-telangiectasia and necrobiosis lipoidica:
an explainable association. Europ. J. Derm. 4: 509-513, 1994. ![]()